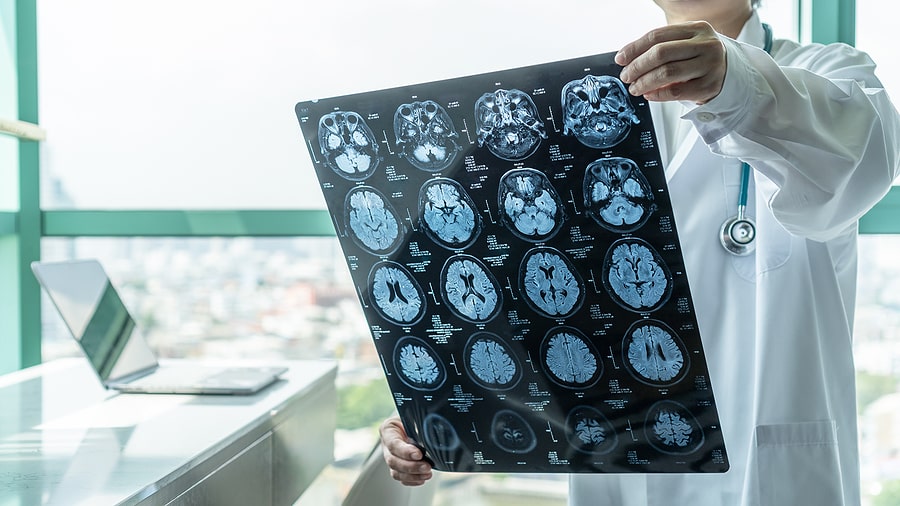
 Traumatic brain injuries affect many more areas of life, from short and long-term memory to coordination, mood, and personality. If you suffered a TBI in an accident due to the negligence of another party, contact an attorney to learn more about your legal rights.
Traumatic brain injuries affect many more areas of life, from short and long-term memory to coordination, mood, and personality. If you suffered a TBI in an accident due to the negligence of another party, contact an attorney to learn more about your legal rights.
How Does Traumatic Brain Injury Occur?
Traumatic brain injury can result from several types of accidents: construction accidents, auto accidents, or slip and fall accidents, for example. While children and older adults are often more prone to traumatic brain injury than those age ranges in between, anyone can suffer traumatic brain injury and its life-altering effects at any age.
Any type of trauma to the head, including a blow, jolt, or bump, can cause a traumatic brain injury. Traumatic brain injury victims may lose consciousness at the scene of the accident, but not all do.
Understanding the Severity of Traumatic Brain Injury
Victims with traumatic brain injury may have a long road to recovery ahead of them. A mild to moderate TBI may leave the victim with symptoms for weeks or even months. In fact, some victims with mild traumatic brain injury may have symptoms more than a year after the initial accident. More severe traumatic brain injury can leave the victim with lifelong symptoms—many of which do not resolve with time. In severe cases, traumatic brain injury can cause the patient to slip into a coma, long-term coma, or death.
Symptoms vary widely depending on the circumstances of the individual. For example, the severity of the symptoms can depend on the severity of the injury suffered or the part of the brain damaged by the traumatic brain injury. With time, traumatic brain injury victims may learn coping mechanisms that can make it easier for them to handle specific situations, which can help alleviate some of the challenges associated with the injury.
Immediate Symptoms of Traumatic Brain Injury
Many victims with traumatic brain injury start showing immediate symptoms at the scene of the accident, especially in the case of a severe TBI. Immediate signs of TBI may include:
- Loss of consciousness. A victim who loses consciousness for even moments should receive a full evaluation from medical professionals, since it could indicate traumatic brain injury.
- A state of confusion. Victims with traumatic brain injury often appear dazed and disoriented at the scene of the accident. First responders may note that they have trouble paying attention to anything happening around them, or that they seem confused.
- Memory gaps. Victims with traumatic brain injury may not remember the accident or the events immediately surrounding it. Often, this memory loss remains even as other symptoms of TBI resolve.
- Nausea or vomiting. Victims may appear physically ill, especially with movement.
- Vertigo. Dizziness and vertigo may result from the trauma to the brain. This symptom may last long-term after the accident or resolve quickly, depending on the severity of the accident and other symptoms.
- Sensitivity to light or sound. Victims may struggle with extreme sensory input, especially at a busy accident scene. Car accident victims, for example, may appear very overwhelmed and struggle to make sense of everything happening around them, especially after moderate to severe TBI.
- Slurred speech or other speech difficulties. Onlookers may mistake symptoms of TBI for drunkenness. The victim may seem overexcited and struggle to get words out. The victim may have slurred speech, making it difficult to understand their speech patterns.
Sometimes, symptoms of TBI go unnoticed at the scene of the accident, especially if the victim does not recall losing consciousness. Even minor accidents, however, can cause a TBI. Any time symptoms appear, the victim should seek medical attention as soon as possible. Family members should also take note if an accident victim seems to sleep much more than usual or appears very difficult to wake. These symptoms could offer evidence of a previously undiagnosed TBI.
Long-Term Symptoms of Traumatic Brain Injury and the Challenges They Present
Victims with even a mild to moderate TBI should expect long-term symptoms and challenges in their lives. Many victims work closely with occupational therapists to help them relearn how to perform common tasks or how to manage some of the difficulties they experience.
Trouble With Focus and Concentration
The brain regulates attention and focus. For some people, focus comes naturally. They may spend hours on a task, single-mindedly moving forward as they work to achieve their goals.
However, for victims with traumatic brain injury, focus and concentration can quickly go out the window. They may struggle to keep their mind on the task at hand, even if they take measures that are usually successful in redirecting the mind and maintaining attention.
This loss of focus and concentration can become detrimental in several areas. First, it can be incredibly frustrating at work, where many tasks rely on sustained focus. Multitasking may seem to be almost impossible, with even the slightest distraction sending the patient’s mind spinning away from the task at hand. Many victims of TBI struggle to finish even short or simple work tasks, especially those that involve sustained attention to detail.
Perhaps more frustrating, for many victims, is that this loss of focus and concentration can make it difficult to enjoy many leisure activities as well. Completing craft projects, reading a book, or even maintaining the focus necessary to watch television can become incredibly difficult. Many victims struggle with the loss of focus associated with traumatic brain injury.
Memory Loss
Many victims with traumatic brain injury do suffer the loss of long-term memories, including memories of loved ones and important events. The events that led up to the accident, in particular, are often incredibly difficult for victims to recall. Memories may come back over time, as the brain heals and forms new pathways.
But sometimes, the victim may permanently lose those memories. The loss of those memories can interfere with relationships and make the victim feel constantly out of step, or as though he or she is “missing something,” even when surrounded by friends and family members. Often, memory gaps show up at unexpected moments, suddenly reminding the victim of everything they lost.
Many traumatic brain injury victims lose short-term memories. Short-term memory, also called active memory, contains the thoughts that the person remains focused on. It includes current tasks: why did you walk into a room? What did you intend to accomplish? What parts of a task have you already finished? It may also include factors like the conversation at hand and the things the person intends to say next; the answer to a question, for example.
Short-term memory has a relatively limited capacity even for healthy individuals. In general, short-term memory has a limited span, and people can only hold an average of seven items (plus or minus two) for any length of time. Victims with traumatic brain injury, on the other hand, may have more trouble maintaining short-term memory and keeping up with everything going on around them. For example, a traumatic brain injury victim might forget the instructions given to them at work before their boss even walks out of the room.
They might go to the supply closet to fetch an item, only to forget where they have already checked; opening the same drawer or cabinet repeatedly. Many victims learn to rely on apps and written instructions to make it easier to maintain these memories. However, these limitations can still make daily functionality more difficult for TBI victims.
Sensory Changes
Changes in sensory perception can make it difficult for victims with traumatic brain injury to navigate the world around them. Some victims struggle with tunnel vision or have blurred vision as a result of their injuries. Others suffer from chronic tinnitus (ringing in the ears), that can interfere with concentration or make it difficult to hear other sounds around them.
Victims with a moderate to severe TBI may also experience significant changes in the way they perceive the world as a whole. Some notice changes to their sense of taste. Their once favorite foods might become undesirable, while foods that they did not previously enjoy might suddenly take on a more pleasant taste. Victims may struggle with changes in the way they perceive heat, cold, or even pain.
These sensory changes can become incredibly disruptive to the victim’s life as a whole. Some sensory changes pose a potent distraction, making life even more difficult for a victim who may already struggle with keeping their mind on the task at hand. Others may experience difficulty functioning, pulling their energy and attention away from the task at hand.
Sleep Disruptions
Traumatic brain injury can permanently change the victim’s sleep habits and the amount of rest needed each day. Some victims with traumatic brain injury may find themselves sleeping considerably more. The increased sleep could result from the brain’s attempt to heal itself. It could also be the result of the mind attempting to escape from the trauma it faces. Other victims struggle to fall asleep at all. Some experience this because they have a fear of falling asleep and the loss of consciousness it brings (particularly after suffering a coma). Some have trouble because the chemistry of the brain simply will not allow them to fall asleep easily.
Sleep disruptions can add to the complications that traumatic brain injury victims face in everyday life. Victims who suddenly require more sleep may need to alter their daily patterns and habits to allow them to get that rest. They may require longer sleep cycles at night, or even need to schedule naps during the day, which can make it difficult for them to handle the other tasks in front of them.
Victims who struggle to sleep, on the other hand, may face additional symptoms. Sleep deprivation can worsen many of the other symptoms associated with traumatic brain injury and make it more difficult for the victim to function. Sleep deprivation quickly interferes with mood, focus, and concentration. It can cause additional difficulties with processing and memory, leaving the victim even more out of sorts than before. Victims may also find that they struggle with a loss of balance or coordination, which can make it more difficult to perform common activities.
Ultimately, sleep disruptions can leave victims struggling with worse symptoms related to the TBI, exacerbating the appearance of the other symptoms and making it difficult for the victim to return to their previous life. Victims may ultimately resort to sleep aids to get enough rest.
Speech Difficulties
Depending on the area of the brain damaged by traumatic brain injury, victims may develop speech disabilities. Some victims may develop a stutter, regardless of whether they had one before. Sometimes, a childhood stutter could reemerge. Speech may appear slurred and difficult to understand. Many victims may struggle to bring the right words to the forefront.
In some victims, this difficulty extends to the written word. For example, victims may struggle to read the words on a page or to clearly communicate concepts through writing.
Speech and communication difficulties can be particularly frustrating for a victim with traumatic brain injury. These speech challenges may make the victim feel lost, alone, and unable to communicate effectively with others. The victim may struggle to clearly explain the challenges they face, the emotions they feel, or their needs. Impaired communication can also create additional relationship challenges, since it can cause a sense of separation between the victim and their loved ones. Some victims do regain the ability to communicate normally over time, while others may struggle with communication challenges for the rest of their lives.
Emotional Difficulties
In addition to the physical effects often associated with traumatic brain injury, many victims suffer from severe ongoing emotional effects. The emotional effects of traumatic brain injury may cause a sense of disconnection in the victim or leave them struggling with the limitations posed by their injuries.
Extreme emotional reactions. In many victims, traumatic brain injury causes extreme emotional reactions. The victim may have an extreme emotional reaction to relatively minor stimuli. For example, in an uninjured individual, a person nearby tapping a pen repeatedly might cause some irritation. In a victim with TBI that impacts the emotions, on the other hand, that pen tapping might cause a bout of extreme rage that is incredibly difficult to control. Likewise, the victim might suffer extreme sadness on finding an empty box of cereal in the cabinet or getting to a much-anticipated movie, only to discover that it sold out or that they misread the show time.
These extreme emotional reactions are not only difficult for victims with traumatic brain injury, they can be extremely difficult for friends and family members who may struggle to navigate those difficult emotional waters and mitigate the extreme emotional responses. In some cases, emotional overreaction can create a wedge between the victim and friends and family members, especially when these reactions tend toward anger.
Depression. The challenges associated with a traumatic brain injury can depress victims who have seen their entire lives changed by their injuries. The “wait and see” approach to learning what comes next can also pose substantial difficulty for many victims who may feel stuck in limbo.
Moderate to severe traumatic brain injury can also trigger depression on its own. Depressed patients may feel hopeless, irritable, or “down.” They may find it difficult to work up enough motivation to tackle the challenges in front of them, or argue that they have no reason to work to overcome those challenges. Depression can make it incredibly difficult for the victim to take on the tasks associated with daily living and responsibilities, much less deal with more complex tasks. Depression can also lead to ongoing aches and pains and sleep disruptions.
In addition, many of the symptoms of depression—including loss of focus and difficulty concentrating—can mimic those already associated with a TBI. Victims with a TBI and depression may notice a worsening of their overall symptoms, and may find it more difficult to overcome them without treating the depression at its source.
Mood swings. Along with the other emotional regulation challenges associated with a TBI, many victims suffer from severe mood swings. One moment, the victim may appear happy, positive, and upbeat, ready to tackle all the challenges in front of him. The next, they may swing to frustration, irritation, or sadness. These mood swings can occur without warning or apparent external stimulus.
These mood swings may interfere with the victim’s daily functioning as well as their relationships with others. Friends and family members may struggle to understand and navigate mood swings, making it difficult for them to interact with the affected individual.
Anxiety. Patients with anxiety often feel restless and wound up. They may struggle to sit still, constantly moving. Anxiety can cause a pervasive feeling of worry, the sense that something has gone wrong, and that the individual can do little or nothing to stop it. Patients with traumatic brain injury may naturally suffer from symptoms of anxiety as they attempt to navigate the world without normal brain function. Depending on the area of the brain impacted by the TBI, the injury itself may also cause increased anxiety.
Victims with TBI-induced anxiety may struggle to get out of the house or to participate in normal activities. They may have an ongoing feeling that people will laugh at them or that they will “mess up” something as they struggle to control their reactions. Anxiety may also make it more difficult for victims with TBIs to try new things, including the coping mechanisms suggested by their doctors or therapists. In extreme forms, anxiety can cause panic attacks and symptoms of PTSD that can make it very difficult for the victim to function in everyday life.
Impulse Control
Most people have some degree of impulse control. It is that voice inside their heads that reminds them that they need to behave appropriately in public or that they should not take certain actions. Some people naturally have less impulse control than others.
Victims with a TBI may have their impulse control stripped away. Often, friends and loved ones do not notice this challenge until weeks or even months after the accident. In some victims, impulse control challenges may seem relatively minor but will pose substantial financial or physical problems later. For example, the victim might struggle with financial responsibility.
They might quickly and repeatedly make purchases that seem to make little sense, including expensive purchases that they cannot afford. In other cases, impulse control challenges can make it very difficult for the victim to avoid saying exactly what they think or doing whatever they want to, regardless of the consequences.
Some TBI victims with impulse control challenges require round-the-clock care to prevent foolish actions that could endanger the victim or others around them. Others may not need constant care, but may lack the control needed to return to work or other normal activities. Impulse control challenges might, for example, make it difficult for a victim to avoid telling a customer exactly what they think of the customer’s demands, despite their role in customer service.
Personality Changes
Some victims with traumatic brain injury suffer from personality changes. For some victims, these changes resolve over time. For others, however, changes occur on a more permanent basis.
Traumatic brain injury can permanently change many elements of a person’s life. An upbeat, generally positive individual may struggle with overcoming the challenges associated with the injury, which can make it more difficult for that individual to function the way they did before the accident. These natural changes often occur alongside serious injuries and life-changing events.
For victims with traumatic brain injury, however, personality changes may appear more stark than that. Some victims suffer a dramatic shift in the way they think, feel about, and deal with the world around them. To the victim, these changes may appear perfectly natural.
Friends and family members, on the other hand, may struggle more with the change. Sometimes, these personality changes turn the victim into a person that their loved ones no longer recognize, or creates personality elements that make them no longer want to spend time with the victim. Other times, these personality differences may become so pronounced that the victim no longer resembles the person they once knew, making it necessary to form new relational ties and interactive patterns with the victim to maintain a relationship.
For the victim with traumatic brain injury, this can be even more traumatic and difficult to manage. The victim may remember former interactions with friends and loved ones and understand that a shift has taken place, but have little idea how to get back to normal.
Complications Associated With a Traumatic Brain Injury
 Suffering a traumatic brain injury causes enough complications in a victim’s life. In some severe cases, however, the victim may suffer more serious complications that can cause further challenges and expenses.
Suffering a traumatic brain injury causes enough complications in a victim’s life. In some severe cases, however, the victim may suffer more serious complications that can cause further challenges and expenses.
Coma
While many victims of traumatic brain injury lose consciousness at the scene of the accident, some stay unconscious longer than others. A long-term coma can leave the victim hospitalized, racking up substantial medical expenses with every day that passes. During a coma, the victim may suffer from muscle atrophy due to an inability to move. A coma victim has no awareness of the world around them, and does not usually respond to external stimuli.
Vegetative State
In extreme cases, traumatic brain injury can cause a vegetative state in the victim. In a vegetative state, the victim may open their eyes, make sounds, or respond to some stimuli, but still appear to have no awareness of the world around them.
Brain Death
In extreme cases, traumatic brain injury can lead to brain death. Brain death occurs when the victim has no brain activity. While the body still functions, the person’s mind is functionally dead. Patients do not come back from brain death.
Seizures
Some victims develop seizures as a result of the trauma to the brain during a TBI. Seizures can appear immediately after the accident or show symptoms months or even years later. During a seizure, an electrical storm in the brain may cause changes in behavior or levels of consciousness. Seizures can cause temporary confusion, staring spells, or jerking in the extremities—depending on the type of seizure and its severity. Many victims find that seizure management has an extreme impact on their daily life.
Victims with uncontrolled seizures cannot drive, and may struggle to maintain regular employment, since seizures can cause ongoing confusion and disorientation immediately after each event. Sometimes, seizures occur due to a specific trigger: flashing lights, a specific smell, or even extreme stress. In other cases, victims may have no idea what triggered the seizure and, therefore, little idea how to avoid the next one.
Headaches
Many victims experience ongoing headaches following a traumatic brain injury. These headaches can range from mild to severe. They may have specific triggers, including extreme stress, or may occur seemingly at random. For some victims, headaches can interfere with the ability to function normally. For others, headaches can require pain medications, which may further increase the symptoms of confusion associated with traumatic brain injury.
Coping Mechanisms for People With Traumatic Brain Injury
Many victims with TBI rely on coping mechanisms to help carry them through their daily lives. Modern technology has offered several options that can make coping with TBI easier, including apps and programs that can aid in both short-term and long-term memory.
For example, victims may find it helpful to use a calendar app to keep track of events and appointments, rather than trying to rely on their faulty memory to keep up with those reminders. Clear schedules can also make life easier for victims with a TBI, since those schedules can remind them of what comes next throughout the day. Other coping mechanisms can be more disruptive to everyday life.
Shortened Tasks
Many victims with traumatic brain injury benefit from breaking tasks down into shorter steps. Sometimes, victims can handle this task on their own. Other times, they may need friends and loved ones to lay out clear instructions, break down tasks, and observe their progress.
Labels and Instructions
Written instructions can make it easier for victims with traumatic brain injury to handle the responsibilities in front of them. They often benefit from visual reminders of how to complete even relatively simple and familiar tasks. For example, a TBI victim might need a list of the items to take with them as they head out the door for the day, or a list of the items in a specific cabinet. Creating these initial lists can be time-consuming, especially if they change often or if the victim’s needs change regularly.
Additional Time and a Safe Space

Because of the frustration and emotional difficulty often associated with a TBI, victims may need additional time and space to deal with tasks. They may also need a safe space they can go to if they have an extreme emotional episode. Some victims may find certain activities impossible for a time after the accident. In extreme cases, victims may never fully regain the ability to participate in all their former activities.
Do You Need a Lawyer After Suffering a Traumatic Brain Injury?
If you suffered a TBI due to the negligence of another party, an attorney can help. Contact an experienced traumatic brain injury attorney to learn more about your legal rights following an accident.
Gomez Trial Attorneys
655 West Broadway, Suite 1700
San Diego, CA 92101
Phone: (619)-237-3490







